What a Midwife Does: Understanding Your Care Options During Labour
A guide to midwifery care in India — what a midwife is, what they do during labour and birth, how midwifery care differs from obstetrician-led care, and where midwives are available in India.
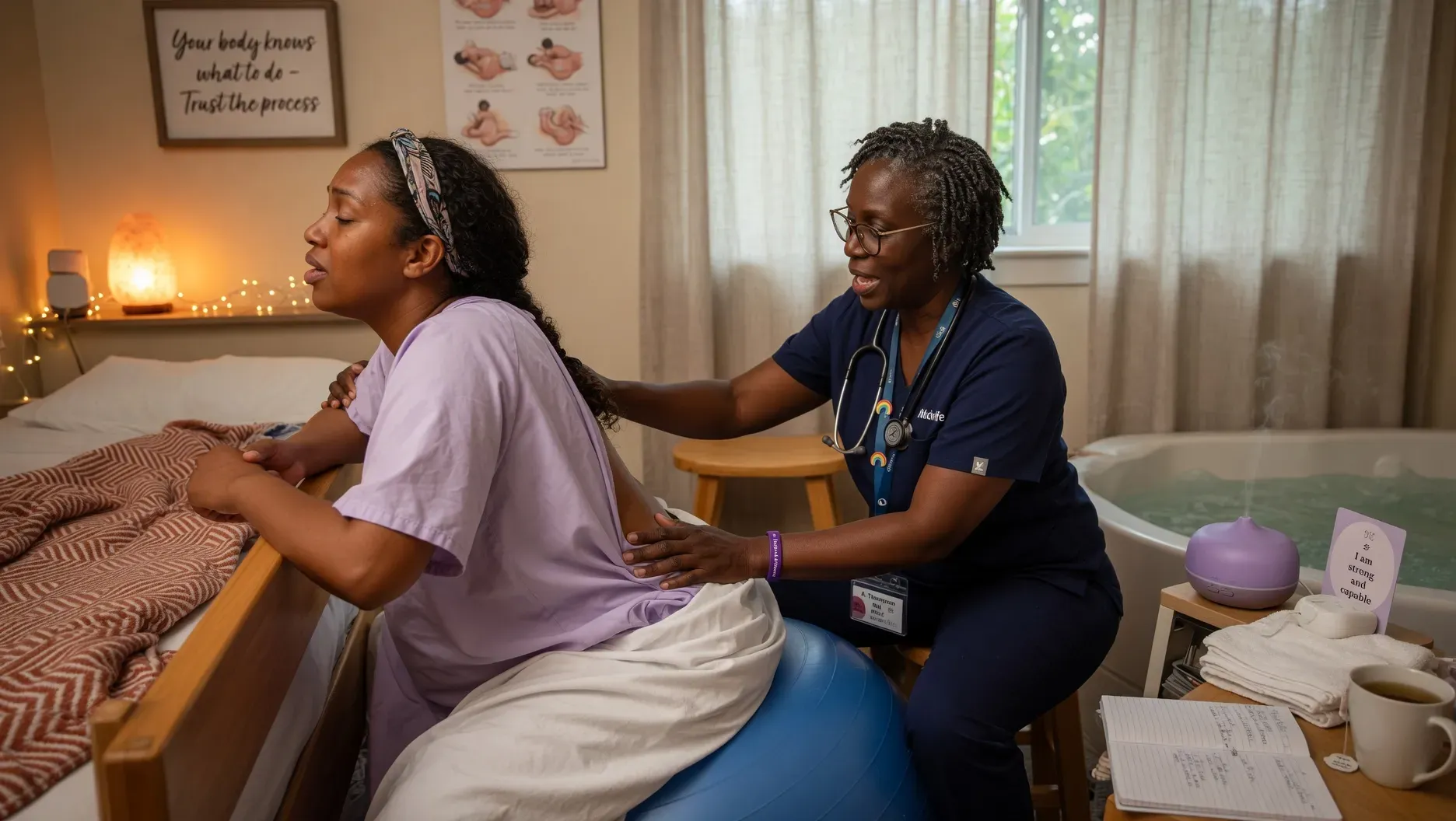
In many countries, midwives are the primary caregivers for low-risk pregnancies and normal births — obstetricians are specialists who become involved when complications arise or when medical expertise is specifically needed. In India, the picture is different and more complex, and many women do not have a clear understanding of what midwives are or what role they play in their care.
This guide explains what midwifery care involves, how it differs from obstetrician-led care, the current state of midwifery in India, and what it means for the choices available to you.
What a midwife is
A midwife is a healthcare professional specifically trained in the care of women during pregnancy, labour, birth, and the postpartum period. Midwifery is a distinct profession from nursing, though in India the two have historically been deeply intertwined — many midwives in Indian hospitals are trained as nurse-midwives, holding qualifications in both nursing and midwifery.
At its core, midwifery is based on a philosophy of birth as a normal physiological process — one that, for the majority of women with healthy pregnancies, does not require medical intervention but does benefit from skilled, continuous, supportive care. This philosophy shapes how midwives approach labour and birth differently from how the obstetrician-led model approaches it.
What midwives do during labour and birth
A qualified midwife providing labour care:
Monitors maternal and fetal wellbeing — regular assessment of vital signs, fetal heart rate monitoring, assessment of labour progress through vaginal examinations, monitoring of contraction pattern and intensity.
Provides continuous support — present throughout active labour, providing physical comfort measures (positioning guidance, massage, breathing support), emotional reassurance, and the particular kind of experienced companionship that makes the difference between a frightening and a manageable labour. Research consistently shows that continuous one-to-one support during labour, provided by a trained support person including a midwife, reduces pain perception, reduces the use of pharmacological pain relief, reduces C-section rates, and improves birth outcomes.
Manages the birth — a trained midwife can manage a normal vaginal birth independently: supporting the woman through pushing, managing the delivery of the baby’s head and body, performing perineal support to reduce tearing, delivering the placenta, and repairing minor tears or episiotomies.
Assesses for complications — part of the midwife’s skill is recognising when a normal process is deviating from the expected course and escalating to medical care appropriately. This recognition and escalation function is central to safe midwifery care.
Provides postpartum care — assessing the mother’s recovery, supporting breastfeeding initiation, monitoring the newborn’s early adaptation.
How midwifery care differs from obstetrician-led care
An obstetrician is a medical specialist — a doctor who has specialised in obstetrics and gynaecology. Their training is focused on diagnosing and managing complications of pregnancy and birth. Obstetricians are the right care provider when things go wrong — when there is a complication requiring surgical or medical intervention, the obstetrician’s expertise is essential.
In the standard Indian model, however, obstetricians are the primary care provider for all pregnancies regardless of risk level — seeing women for antenatal appointments, attending the birth, and managing normal deliveries as well as complicated ones. This is partly a reflection of the shortage of qualified midwives relative to the birth rate, and partly a cultural and professional dynamic in which obstetric-led care has become the norm.
The difference in approach is not simply about who is in the room. Midwifery-led care for low-risk pregnancies is associated with higher rates of spontaneous vaginal birth, lower rates of episiotomy, lower rates of instrumental delivery, higher rates of breastfeeding initiation, and higher maternal satisfaction — while maintaining equivalent safety outcomes to obstetrician-led care for women without risk factors.
This is not an argument that obstetricians provide inferior care. It is an argument that the skills each professional brings are suited to different aspects of the care continuum, and that the integration of skilled midwifery care into the system improves outcomes for normal births.
The state of midwifery in India
India has a significant midwifery workforce, but historically it has operated in a subordinated nursing role rather than as an autonomous profession. The typical “staff nurse” in an Indian government hospital maternity ward is often a trained nurse-midwife managing much of the practical labour care, but without the professional recognition, autonomy, or scope of practice that midwives hold in countries where midwifery is a recognised standalone profession.
The National Midwifery Policy Framework (2018) and subsequent efforts to establish a cadre of Nurse Practitioners in Midwifery (NPM) represent a significant shift — a government-led effort to train and deploy a new generation of qualified midwives with the skills and professional recognition to provide autonomous care for normal births.
Midwifery-led birth centres are beginning to emerge in some Indian cities — typically attached to larger hospitals but providing a less medicalised environment for low-risk births supported by qualified midwives. These are currently concentrated in urban areas and are not yet widely available.
ASHA workers and trained birth attendants (TBAs) in community and rural settings provide a different form of maternity support — important for access in areas without institutional facilities, but distinct from the clinical role of a qualified midwife.
What this means for your care
For most women delivering in Indian hospitals in 2026, the immediate care during labour will be provided by nurses — many of them with midwifery training — with obstetrician oversight and involvement at key points including the actual birth.
The practical implications for your care:
- The nurse assigned to you in the labour ward plays a significant role in your experience. A skilled, attentive nurse-midwife who provides continuous support makes a genuine difference to labour outcomes.
- Asking for continuous support — from a nurse, a partner, a family member, or a doula if available — is one of the most evidence-supported choices you can make for your birth.
- If you are in a city where midwifery-led birth centres are available and your pregnancy is low-risk, this is a genuinely different and often more supportive care model worth exploring.
- Wherever you deliver, the relationship between you, your doctor, and the nursing team — built on communication and mutual respect — shapes the quality of your birth experience as much as the facility itself.
This article is for general educational purposes only. The availability of midwifery care varies significantly by location and facility in India. Discuss your care options with your healthcare provider.