What Is a Normal Labour Timeline: First Baby Versus Subsequent Pregnancies
A clear guide to what a normal labour timeline looks like — the stages of labour, typical durations for first and subsequent babies, and what influences how long labour takes.
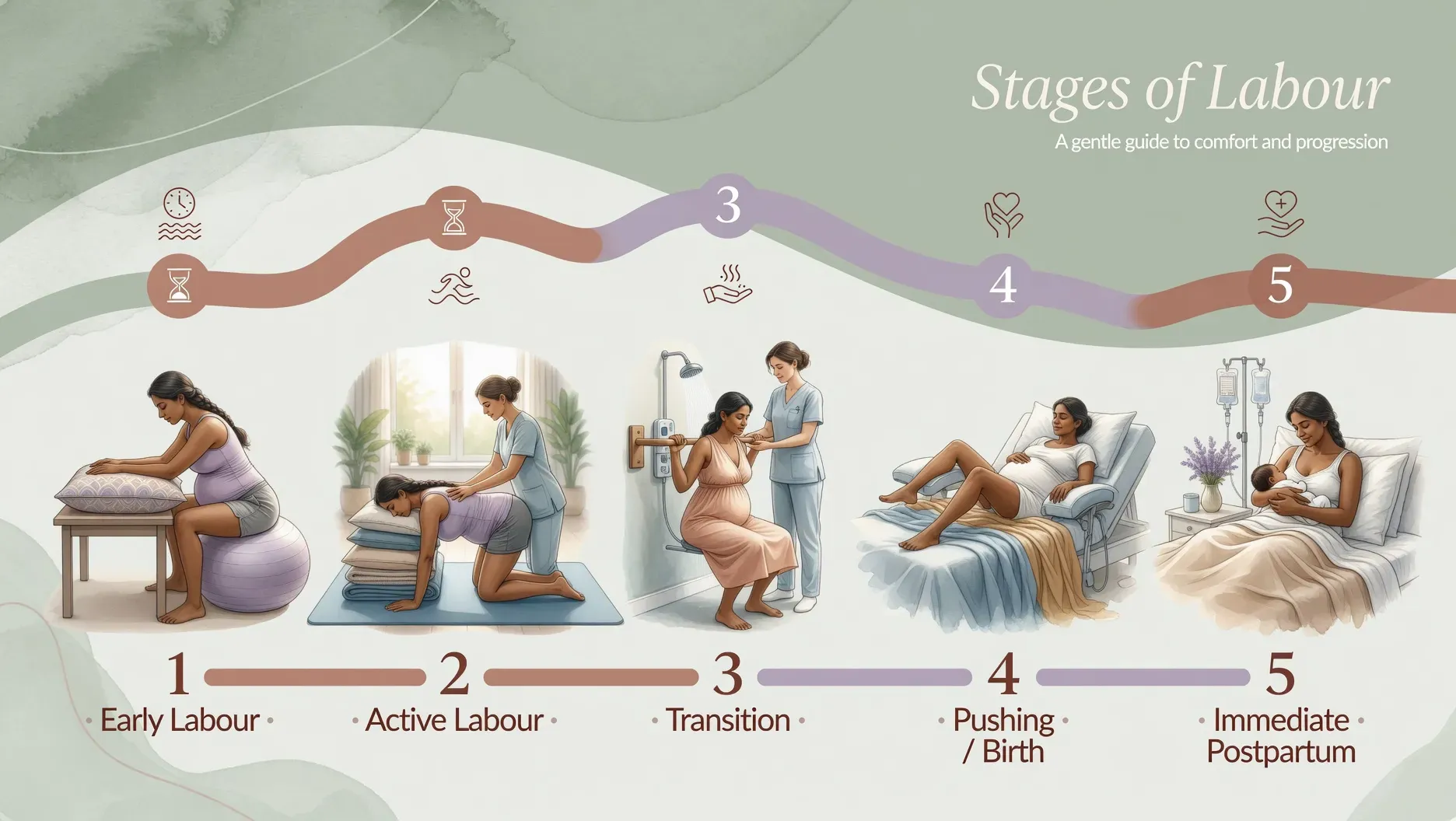
Labour has a well-established structure — three stages, each with typical characteristics and typical durations — but the timeline within that structure varies considerably between individuals and between first and subsequent pregnancies. Understanding what is typical, what is normal variation, and what represents a deviation from normal helps you arrive at labour with realistic expectations rather than the anxiety of not knowing what the experience is supposed to look like.
The three stages of labour
First stage: From the onset of regular labour contractions to full cervical dilation (10cm). This is by far the longest stage and is further divided into early labour and active labour.
Second stage: From full dilation to the birth of the baby.
Third stage: From the birth of the baby to the delivery of the placenta.
First stage: early labour
Early labour begins when contractions become regular and progressive — increasing in length, strength, and frequency — and ends when the cervix has dilated to approximately 6cm. During this phase, the cervix both dilates (opens) and effaces (thins).
What it feels like: Contractions that are noticeable but usually manageable — discomfort that is present but not yet overwhelming. They begin irregularly and gradually establish a more consistent pattern. Some women describe them as strong period pain; others feel them primarily as lower back pressure.
Typical duration — first baby: 6–12 hours, sometimes longer. Early labour is unpredictable and highly variable. Some women spend a significant portion of this phase at home or moving around, others progress quickly into active labour.
Typical duration — subsequent pregnancies: Often shorter — 2–6 hours in many cases, though again with significant variation. The cervix of a woman who has given birth before tends to dilate more efficiently.
What to do: Most providers recommend staying home during early labour, staying hydrated, eating if you feel able, resting, and keeping your support person informed. The hospital is not usually necessary until active labour is established.
First stage: active labour
Active labour begins at approximately 6cm dilation and continues to full dilation at 10cm. This is the phase of more intense contractions, typically 3–5 minutes apart and lasting 45–60 seconds.
What it feels like: Contractions that require active coping — you cannot talk through them in the way you could in early labour. Many women find breathing techniques, movement, warmth, massage, or a support person’s presence most helpful in active labour.
Typical duration — first baby: 4–8 hours. Active labour progression is measured clinically as approximately 0.5–1cm of dilation per hour, though this is a guide rather than an exact expectation.
Typical duration — subsequent pregnancies: 2–4 hours is common. Subsequent labours are generally faster, particularly in active labour.
Transition: The final part of active labour — from approximately 8cm to full dilation — is often the most intense period. Contractions are long, strong, and very close together. Many women feel overwhelmed, may feel they cannot continue, or feel a strong urge to push before full dilation is reached. This phase is typically the shortest — 30 minutes to 2 hours — but emotionally the most demanding.
Second stage: pushing and birth
From full dilation to the birth of the baby. Once the cervix is fully dilated, the pushing phase begins — either with your body’s spontaneous urge or, in some hospital settings, with directed pushing guided by the care team.
Typical duration — first baby: 1–3 hours, though significant variation exists. Some women push for less than 30 minutes; others push for longer with appropriate monitoring.
Typical duration — subsequent pregnancies: Often much shorter — 20 minutes to 1 hour is common for women who have given birth vaginally before.
What influences second stage duration: The baby’s position (facing backward — occiput anterior — is easiest; facing forward — occiput posterior — typically requires longer pushing), the baby’s size, the mother’s position during pushing (upright, squatting, or on hands and knees tend to be more efficient than lying on the back), and the effectiveness of the pushing effort.
Third stage: delivery of the placenta
After the baby is born, the uterus continues to contract to separate and deliver the placenta. This stage is covered in more detail in a separate guide.
Typical duration: 5–30 minutes with active management (an injection of oxytocin given after birth to speed placental separation, standard in most Indian hospital settings). Without active management, it may take up to an hour.
What makes labour longer
- First pregnancy (the cervix has not dilated before)
- Posterior baby position (occiput posterior)
- Induction of labour (contractions may take longer to establish effective dilation compared to spontaneous labour)
- Epidural (can slow active labour progression in some cases)
- Dehydration and fatigue
- High anxiety and muscle tension
What makes labour faster
- Subsequent pregnancy
- Optimal baby position (occiput anterior)
- Upright and active positioning during labour
- Good hydration and nutrition in early labour
- Effective support from a birth partner or doula
- Calm environment and reduced anxiety
When labour is considered prolonged
Prolonged labour — failure to progress — is one of the most common reasons for medical intervention during labour. The definitions vary, but in general: active labour that does not progress at approximately 0.5cm per hour, or a second stage that extends beyond accepted limits without continued progress, may prompt discussion of augmentation (oxytocin to strengthen contractions), instrumental delivery (forceps or vacuum), or caesarean section.
These interventions exist for good reasons and have significantly improved birth outcomes. Understanding when they are likely to be raised — and why — helps you participate in the decision rather than simply receive it.
This article is for general educational purposes only. Labour varies enormously between individuals, and your specific experience will be guided by your care team based on your individual circumstances.