What Happens in the Third Stage of Labour: Delivering the Placenta
A clear guide to the third stage of labour — what it is, active versus physiological management, what to expect, and why it matters for postpartum bleeding risk.
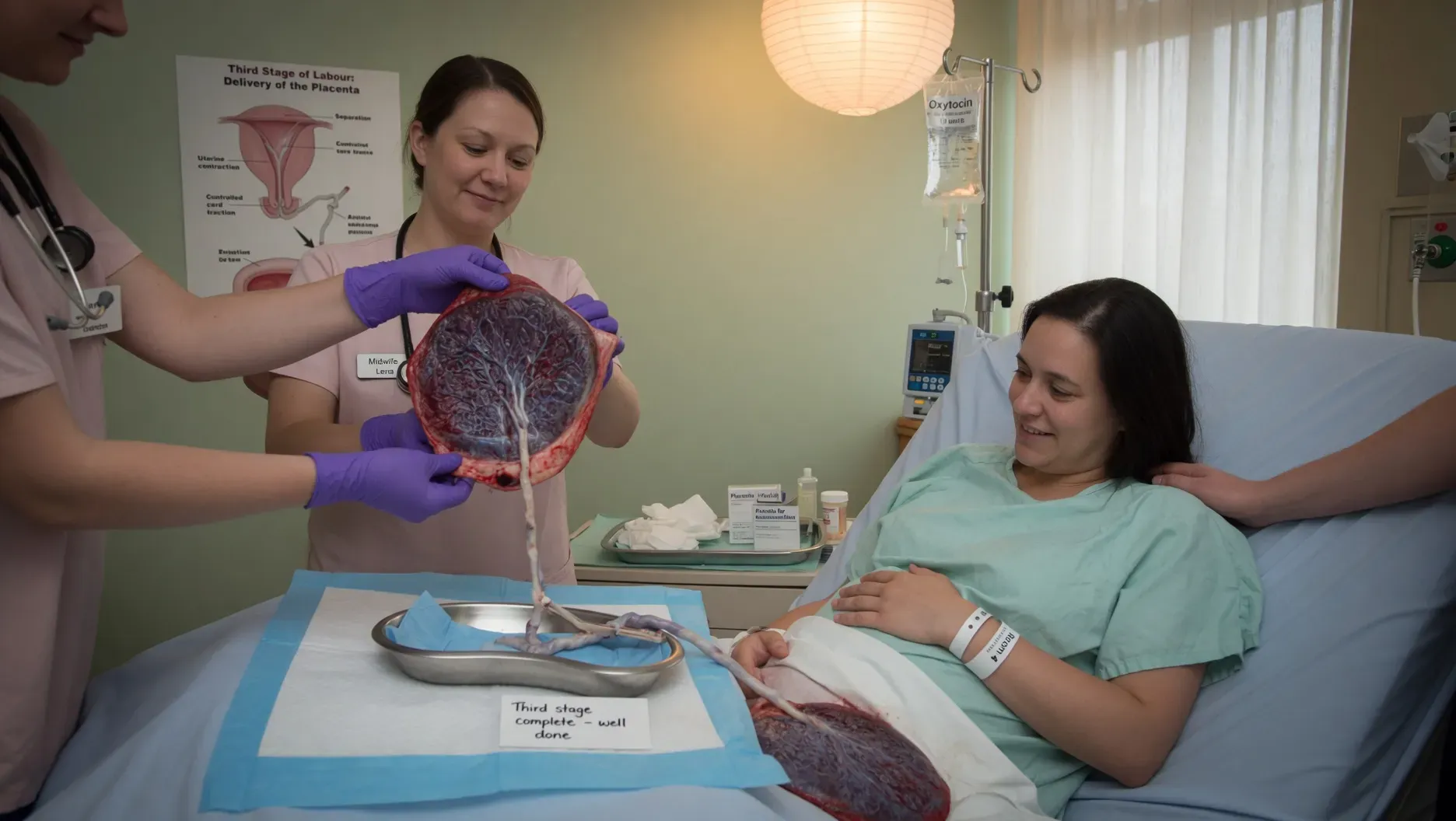
The third stage of labour is the period after the baby is born and before the placenta is delivered. It is the shortest of the three stages and the one that receives the least preparation from antenatal care — most birth preparation focuses on labour and the birth of the baby, and the placenta is something many women find themselves unprepared for.
Understanding what happens in the third stage, the difference between managed and physiological approaches, and the warning signs of complications gives you a complete picture of the birth process rather than an experience that ends abruptly with the baby and continues, confusingly, without preparation.
What the placenta is
The placenta is the extraordinary organ that grew from the same fertilised egg as your baby — an entirely new organ created during pregnancy to serve as the interface between your circulation and your baby’s. It transfers oxygen and nutrients, removes waste products, produces pregnancy hormones, and provides immune protection. It has been sustaining your baby’s life for nine months and typically weighs approximately 500–600g at term.
After the baby is born, the placenta has completed its function. The uterus contracts to separate the placenta from the uterine wall, and the placenta is expelled through the cervix and vagina.
Active management versus physiological management
The third stage can be managed in two ways, and most Indian hospitals use active management as standard.
Active management involves an injection of oxytocin (usually given into the thigh or IV) immediately after the baby’s birth, controlled cord traction (the midwife or doctor applies gentle traction to the umbilical cord while the other hand supports the uterus to guide the placenta out), and early cord clamping in some but not all protocols.
Active management significantly reduces the risk of postpartum haemorrhage — heavy bleeding after birth — which is one of the leading causes of maternal mortality in India. For this reason, it is standard practice in most Indian hospitals and is the recommended approach by the WHO for all births in healthcare facilities.
Physiological management involves allowing the uterus to contract and expel the placenta naturally, without medication or cord traction, waiting for the placenta to separate and deliver on its own — which typically takes 20–60 minutes. This is less commonly used in Indian hospitals and is associated with higher postpartum haemorrhage risk in facility-based settings.
Delayed cord clamping — allowing the umbilical cord to stop pulsating (typically 1–3 minutes after birth) before clamping and cutting — can be incorporated into active management and transfers additional blood volume and iron to the baby. If this is something you want, include it in your birth plan discussion with your doctor.
What the experience is like
While the baby is being assessed, warmed, or placed on your chest for skin-to-skin, the care team will be attending to the third stage. The oxytocin injection is given almost immediately after birth — you may not notice it in the context of everything else happening.
You will be asked to push once more when the placenta has separated — there will be a feeling of pressure and a brief, usually easy expulsion. The placenta does not feel like delivering the baby — it is softer and usually comes out within a few pushes without significant effort or pain.
If the placenta does not deliver within 30 minutes with active management, this is called a retained placenta and requires further intervention — sometimes manual removal, occasionally surgical.
After the placenta is delivered, your doctor or midwife will examine it to confirm that it is complete — that no fragments remain in the uterus, which would cause bleeding and infection.
Postpartum haemorrhage — the risk the third stage manages
Postpartum haemorrhage (PPH) — heavy bleeding after birth — occurs when the uterus does not contract effectively after delivery. The contracting uterus squeezes the blood vessels that supplied the placenta; if it does not contract properly, those vessels remain open and bleeding continues.
Active management of the third stage with oxytocin reduces PPH risk significantly. Risk factors for PPH include: a long labour, very large baby, multiple pregnancy, placenta previa, previous PPH, and certain blood clotting conditions.
If you experience unusually heavy bleeding after birth, the care team will act quickly — additional medications to contract the uterus, IV fluids, and in some cases surgical intervention are the management steps. Knowing that this is a managed complication rather than a crisis requiring panic is useful.
This article is for general educational purposes only. Discuss the management of your third stage, including your preferences around cord clamping, with your obstetrician before your due date.